Abstract
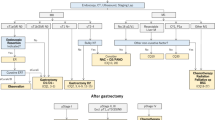
Clinical practice guidelines for gynecologic cancers have been published by the National Comprehensive Cancer Network and the National Cancer Institute. Whereas these guidelines form the basis for the standard of care for gynecologic malignancies in the United States, it has proven difficult to institute them in Japan due to differences in patient characteristics, health-care delivery systems, and insurance programs. Therefore, evidence-based guidelines for treating cervical cancer specifically in Japan have been under development. The Guidelines Formulation Committee and Evaluation Committee were independently established within the Committee for Treatment Guidelines for Cervical Cancer. Opinions from within and outside the Japan Society of Gynecologic Oncology (JSGO) were incorporated into the final draft, and the guidelines were published after approval by the JSGO. These guidelines are composed of ten chapters and comprise three algorithms. Each chapter consists of a clinical question, recommendations, background, objectives, explanations, and references. The objective of these guidelines is to clearly delineate the standard of care for cervical cancer treatment in Japan in order to ensure equitable care for all Japanese women diagnosed with cervical cancer.



Similar content being viewed by others
References
Ushijima K (2009) Current status of gynecologic cancer in Japan. J Gynecol Oncol 20(2):67–71
Pearcey R, Miao Q, Kong W et al (2007) Impact of adoption of chemoradiotherapy on the outcome of cervical cancer in Ontario: results of a population based cohort study. J Clin Oncol 25:2383–2388
Acknowledgments
We thank the Japan Society of Obstetrics and Gynecology, Japan Association of Obstetricians and Gynecologists, Japanese Gynecologic Oncology Group, and Japan Society of Clinical Oncology for their comments and contributions throughout the project.
Conflict of interest statement
K. Fujiwara has employment with Zeria Pharmaceuticals and received honoraria from Bristol-Myers Squibb, Sanofi Aventis, Yakult Honsha, Janseen Pharmaceutical and Zeria Pharmaceuticals. K. Fujiwara also received research funding from Sanofi Aventis, Kaken Pharmaceutical, and Nippon Kayaku. K. Ochiai received honoraria from Taiho Pharmaceutical and research funding from Bristol-Myers Squibb and Chugai Pharmaceutical. No other author has a conflict of interest.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Nagase, S., Inoue, Y., Umesaki, N. et al. Evidence-based guidelines for treatment of cervical cancer in Japan: Japan Society of Gynecologic Oncology (JSGO) 2007 edition. Int J Clin Oncol 15, 117–124 (2010). https://doi.org/10.1007/s10147-010-0061-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-010-0061-x